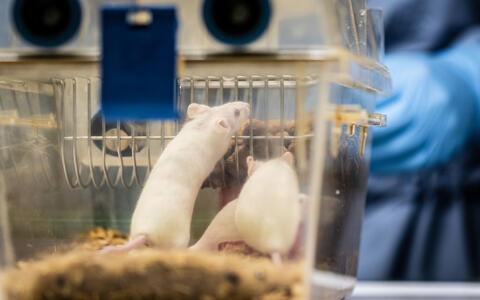
Interpretation of EU animal welfare directive needs to be revised
Immunologist Dr. Thomas Kammertöns’ research at the Max Delbrück Center for Molecular Medicine in the Helmholtz Association (MDC) and Charité – Universitätsmedizin Berlin includes investigating new immunotherapies against cancer. To understand the mechanisms of the immune system, he works with animal models like mice. It is true that many questions in biomedicine can now be answered using alternatives to animal experiments – such as computer models, organs-on-a-chip, and organoids. But hardly any other system in the body is as complex as the immune defense system. A vast network of immune cells carried via blood and lymph vessels spans all of our organs. This network is in constant communication with all the body’s cells, monitoring them and intervening whenever it senses a threat.
Even SARS-CoV‑2 vaccines would not exist today without decades of basic research into mRNA vaccines – which include experiments on mice with genetically modified immune systems.
“If we want to penetrate this complexity, we are dependent on animal experiments,” says Kammertöns. “This is the only way we can hope to develop therapies against cancer and investigate autoimmune diseases and viral infections. Even SARS-CoV‑2 vaccines would not exist today without decades of basic research into mRNA vaccines – which include experiments on mice with genetically modified immune systems.”
The keeping of genetically modified animals has been a topic of debate for many years. It is regulated by the EU directive on the protection of animals used for scientific purposes adopted in 2010 (2010/63/EU). This directive stipulates that scientists must submit an application to the competent regulatory authority if they wish to breed genetically modified animals in a way that may adversely affect the welfare of the animals – i.e., that may subject them to pain, suffering, distress or lasting harm. In its 2013 “Working document on genetically altered animals,” developed to facilitate the implementation of the directive, an EU Expert Working Group determined that merely the risk of such adverse effect constitutes a burden for the animals, thus making project authorization necessary. At the same time, it categorized all genetically immune-modified animals as being at increased risk of infection.
- Avoiding unnecessary animal studies
-
There is a consensus in the research community that animal experiments should only be carried out as a last resort, while minimizing the adverse impact on research animals and improving their housing and husbandry. The guiding concept here is the “3R principles,” which were outlined by the zoologist William Russell and the microbiologist Rex Burch in their 1959 book The Principles of Humane Experimental Technique. The 3Rs stand for replace, reduce and refine. The competent regulatory authority will only approve an animal experiment if the scientists, animal facilities and institutions involved implement the 3R principles. This means the experiment will not be allowed to take place if there is an alternative method to achieve the desired scientific objectives (replace). If it does take place, researchers may only use the indispensale number of animals (reduce), and the experiment must be designed so that the animals experience as little pain, suffering, distress or harm as possible (refine).
Learn more: The 3R principles
Red tape that helps neither research nor animals
Since then, scientists who need immune-modified respectively immunodeficient animals for their research have not only had to submit applications to conduct their experiments – they are also required to have a permit to breed and keep the animals in the first place. “But from an immunological point of view, the blanket assumption that these animals are burdened from the outset is simply not valid,” says Kammertöns.
In Animals, he and his co-authors argue that instead of classifying all immunodeficient animals as “burdened” by this state, the actual burden caused should be assessed on a case-by-case basis. Their argumentation is not purely from an immunological perspective, but also includes insight from ethical and legal experts, laboratory animal scientists and animal welfare officers – who serve as “advocates” for the animals themselves. Kammertöns’ co-authors are veterinarian and MDC animal welfare officer Dr. Sarah Jeuthe; ethicist Dr. Heike Baranzke, who teaches moral theology at the University of Wuppertal; Antonina Klippert, an animal welfare officer at the Nuvisan Innovation Campus Berlin; and Professor Christa Thöne-Reineke, a veterinary specialist of laboratory animal science and physiology, an animal welfare officer, and head of the Institute of Animal Welfare, Animal Behavior, and Laboratory Animal Science at Freie Universität (FU) Berlin.
In PLOS ONE, Berlin scientists report that immunodeficient and healthy mice behave in exactly the same way in pathogen-free housing conditions.
The authors of the “Working document on genetically altered animals” cite the specific-pathogen-free (SPF) conditions under which immunodeficient animals are kept as evidence of them being at higher risk of infection – and thus of the presumed burden that needs to be avoided. “However, SPF animal housing is a necessary condition for research – its primary function is not to reduce the burden on the animals,” explains Kammertöns. In recent years, the immunologist has repeatedly studied the well-being of immunodeficient animals in pathogen-free housing conditions. In 2020, a study was published in the journal PLOS ONE in which Kammertöns, together with first author Sarah Jeuthe and colleagues from FU and Charité, investigated the behavior and physiology of 90 laboratory mice for nine months. They found that the immunodeficient mice did not fare any differently than the healthy mice in the control group.
- Immunodeficiency does not put a strain on mice
-
The scientists report in PLOS ONE that immunodeficient and healthy mice behave in exactly the same way in a pathogen-free environment: They weigh the same, their fur contains the same amount of the stress hormone cortisol, and they also exhibit the same burrowing and nest building behavior. “Mice that feel well build a complex nest and organize the cage, they make themselves cozy,” explains Christa Thöne-Reineke of the FU. “Mice that aren’t doing well behave differently and stop keeping their cage tidy.” Only during the observation of facial expressions according to the international standard of the Mouse Grimace Scale, did a few mice show slight signs of discomfort. The presence of humans alone, however, is enough to cause the mice to narrow their eyes or pull back their whiskers (also known as vibrissae or tactile hairs). Thöne-Reineke’s team developed the behavioral protocol that Kammertöns’ team used for the study at the Berlin-Brandenburg research platform BB3R. Similar to the Charité’s Einstein Center 3R, the platform aims to support the establishment of alternative and animal-friendly methods in biomedical research.
Learn more: Immunodeficiency does not put a strain on mice kept in pathogen-free environments
A pathogen-free environment is “good scientific practice”
Furthermore, the breeding and keeping of laboratory animals under SPF conditions is not reserved solely for those with immunodeficiencies. The Federation of European Laboratory Animal Science Association (FELASA) considers these conditions to be “good scientific practice” for all laboratory animals – regardless of whether researchers have genetically modified their immune systems or not. Modern animal housing facilities are subject to the strictest hygiene regulations. For example, each individual cage has its own ventilation system so that the animals cannot infect each other, and all animal keepers and scientists who come into contact with the animals must first prepare themselves as surgeons would for an operation. This is to protect the animals from any non-experimental diseases – which is for their own well-being, but also ensures the researchers obtain comparable results that have not been distorted by other pathogens.
We want to maximize animal welfare. But when bureaucratic formalities confuse scientists and do nothing for the animals, we have to question their purpose.
According to Kammertöns, this alone disproves the higher risk of infection that the EU Expert Working Group fears for immunodeficient animals. “Firstly, it is highly unlikely that these animals are going to come into contact with pathogens in modern animal facility conditions – conditions that, it must be stressed, apply to all laboratory animals,” explains the scientist. “Secondly, modifying the immune system does not necessarily result in a higher susceptibility to any particular pathogen.” In fact, he explains, sometimes the opposite is true: If lab mice with unmodified immune systems are infected with Leishmania – parasites transmitted to vertebrates by mosquitoes – they perish. But in immunodeficient mice where a specific receptor has been switched off, this infection is no longer fatal. “The particular immune response is always determined by a combination of the animal’s genetic background and the pathogen type,” says Kammertöns. “So the simple fact that the immune system has been modified does not automatically entail a higher risk of infection. If there’s no risk of infection, there’s no burden on the animal. And if there’s no burden on the animal, the project should not require authorization.”
Questioning the formal requirements
Together with his co-authors, Kammertöns is making an urgent plea to abolish the blanket definition of what constitutes a burden and the authorization currently required for immunodeficient animals. “We do not want to compromise the well-being of the laboratory animals,” emphasizes Thöne-Reineke. “We want to maximize animal welfare. But when bureaucratic formalities confuse scientists and do nothing for the animals, we have to question their purpose.” The scientists are calling instead for an individual severity assessment to be carried out on every line of immunodeficient mice. In addition, they want the European Commission to reconsider its stance on SPF animal housing conditions and recognize that this is not a “refinement” – i.e., a measure taken to minimize the burden on the animals – but is in fact the worldwide accepted standard in experimental animal husbandry.
Text: Jana Ehrhardt-Joswig
Further information
- Immunodeficiency does not put a strain on mice kept in pathogen-free environments
- Transparency Agreement for Animal Research launched
- Thomas Sommer on the animal testing transparency initiative
- Mini-organ, mathematical model or mouse?
- A milestone in making experiments more animal friendly
- Research, animal experiments and the 3Rs
Literature
Kammertöns, Thomas et al. (2021): „Breeding and Maintenance of Immunodeficient Mouse Lines under SPF Conditions — A Call for Individualized Severity Analyses and Approval Procedures“. Animals, DOI: 10.3390/ani11061789
Jeuthe, Sarah et al. (2020): „Stress hormones or general well-being are not altered in immune-deficient mice lacking either T- and B- lymphocytes or Interferon gamma signaling if kept under specific pathogen free housing conditions“. PLOS ONE, DOI: 10.1371/journal.pone.0239231