Tackling rare kidney diseases
When the body comes into contact with viruses, bacteria, or other pathogens, the complement system is one of the front lines of defense in fighting these foreign invaders. It forms part of our innate immune system and consists of more than 30 proteins circulating in the blood. Sometimes, however, this patrol unit can be a little overzealous. “This can result in a number of complications, including two rare kidney diseases: atypical hemolytic uremic syndrome, or aHUS, and complement 3 glomerulopathy, or C3G,” explains Professor Michael Bader, who heads the Molecular Biology of Peptide Hormones Lab at the Max Delbrück Center.
As part of the European Joint Programme on Rare Diseases, Bader’s lab and six other research groups from six European countries have now received a grant of more than €1.9 million in total – €300,000 of which will go to the Max Delbrück Center. The researchers will use this money to develop new techniques that will assist in the early and accurate diagnosis of these diseases, and help improve treatment options. The COMPRare project, which will last three years, will be coordinated by pediatric nephrologist Professor Nicole van de Kar of Radboud University Medical Center in Nijmegen, the Netherlands.
Acute and chronic kidney damage
There are a number of tests available, but they vary widely from lab to lab. We want to develop precise and standardized assays.
Patients with aHUS experience inflammation of the kidneys accompanied by blood clot formation in the smallest blood vessels, the capillaries, which can lead to sometimes life-threatening circulatory complications. C3G, on the other hand, involves a buildup of complement fragments in the kidneys. Both diseases are known to damage the kidneys. “Inhibiting the complement system is already the therapy of choice for aHUS, and could also have great potential in the treatment of CG3,” says Bader. This is being demonstrated, he explains, by a growing number of large-scale clinical trials of complement-inhibiting drugs.
“However, it is still a challenge for doctors to diagnose the disorders quickly and accurately,” explains Bader. So, one of the goals will be to identify genetic variants in the complement proteins that are typical of aHUS. “There are already a number of tests available, but they vary widely from lab to lab,” says Bader. “We want to develop precise and standardized assays.”
Searching for biomarkers
Currently, there is also no consensus on the duration and optimal dosage of monoclonal antibody therapy. The researchers therefore want to develop new biomarkers and protocols to monitor and predict disease progression in aHUS and CG3 patients. And they plan to search for previously unknown molecules that influence the complement system – and thus also the development and progression of the two kidney diseases. “Such molecules could serve as both biomarkers and therapeutic targets,” says Bader.
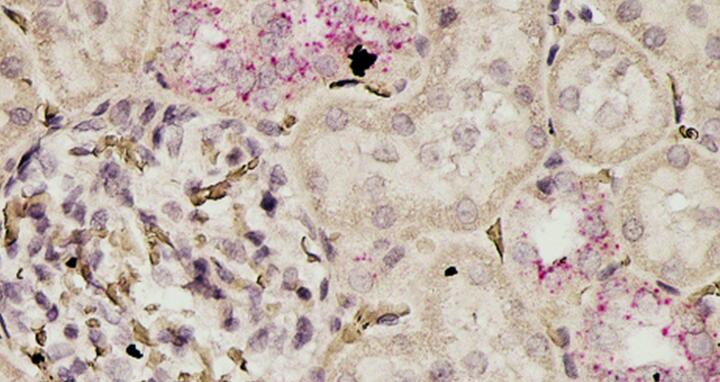
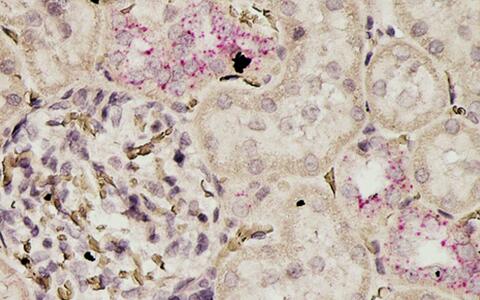
The enzyme carboxypeptidase M (marked in red) inhibits a unit of the immune defense in the kidney that can be overactive. The image shows a cross-section of the tubules and of a filtration corpuscle (glomerulus) in the kidney of a rat.
He will be focusing on the renin-angiotensin system and the kallikrein-kinin system. The former is used by the body to regulate fluid and electrolyte levels as well as blood pressure, while the latter is made up of several proteins in the blood. It is still poorly understood why these particular proteins influence blood pressure and blood clotting, as well as inflammation and pain. “We do not yet know whether and to what extent the kallikrein-kinin system is involved in these two kidney diseases,” says Bader, but adds that certain experiments conducted by partners suggest it may play a role in the activation of the complement system. “We will examine this question with the help of animal models,” he reports.
A potential therapeutic avenue for COVID-19
He also has another protein in his sights: the enzyme carboxypeptidase M (CPM), which sits on the surface of cells. “The two most important systems targeted by this enzyme are the kallikrein-kinin and complement systems,” explains Bader. “We know, for example, that CPM inhibits the complement system in the kidneys.” According to Bader, this could also be of interest for COVID-19 research: “A lot of the damage caused by SARS-CoV-2 could very well be traced back to an overactive complement system in the respective organ,” says the scientist. Thus, CPM may also play a critical role in more common diseases that involve the complement system: “By using therapeutic agents that activate this enzyme, it may be possible to prevent damage not only to the kidneys, but to many other organs as well,” says Bader.
Text: Anke Brodmerkel