A window onto the brain (and more)
It is usually ophthalmologists who examine the retina in the fundus of the eye, such as when they suspect retinal detachment or age-related macular degeneration. But the retina contains not only light-sensitive cells but also complex networks of nerve cells and a web of capillaries. Dr. Hanna Zimmermann, who long worked under Prof. Friedemann Paul at the Experimental and Clinical Research Center (ECRC) – a joint institution of Charité – Universitätsmedizin Berlin and the Max Delbrück Center for Molecular Medicine – is now doing research on the visual system as a junior professor with her own lab. The professorship is endowed by the Einstein Center Digital Future. Hanna Zimmermann’s goal is to use changes in the retina to draw inferences about diseases of the brain and other organs. Her particular focus is on neurological and cardiovascular diseases.
Dr. Hanna Zimmermann.
Multiple sclerosis (MS) is an example of a disease for which the retina is a good marker. Inflammation of the optic nerves is a common sign. As Zimmermann, who has been working with MS patients for several years now, explains, “It leads to visual impairments that are often the first symptom of MS.” Inflammation of the optic nerves causes a thinning of retinal neuronal layers. “But in some patients, the neuronal layers become thinner without any subjective visual impairment. That’s a risk factor for severe disease progression,” Zimmermann added, noting as well that this information is also helpful when assessing the costs and benefits of various treatment options.
Dynamic vascular analysis is a promising method
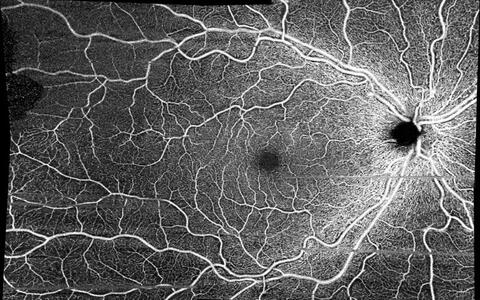
To examine blood vessels in the retina, Zimmermann has established methods like dynamic vascular analysis. This entails stimulating the retina with flashing lights, causing the diameter of the blood vessels to change. “It allows us to draw inferences about the functioning of the internal vessel lining. There is evidence to suggest that it is impaired in patients with post-COVID fatigue,” Zimmerman says. Another promising method is optical coherence tomography angiography, which provides a statistical measurement of vascular density and branching.
In the future, Zimmermann will focus on risk assessment for various vascular diseases. “We aim to establish new methods for identifying certain phenotypes in the retina. We also plan to use artificial intelligence to find parameters that can serve as prognostic markers of disease progression.”
When retinal scans become routine
Ideally, this would allow characteristic patterns to be recognized before a disease manifests. Retinal scans could thus someday become part of a routine physical examination performed by a general practitioner – for the early recognition of neurogenerative disorders, heart and vascular diseases, and renal dysfunction.
The retinal scan could become part of the routine check-up with the family doctor. It is used for early detection of neurodegenerative diseases, cardiovascular diseases or even kidney dysfunction.
Zimmerman’s scientific interest in the retina dates back to her early career. In 2009, while pursuing a degree in medical technology at the Berliner Hochschule für Technik (then called Beuth University of Applied Sciences), she studied retinal changes in MS patients as a student assistant in Friedemann Paul’s Clinical Neuroimmunology Group at the NeuroCure Cluster of Excellence. “It was cutting edge at the time, and I was there from the beginning.” She then wrote her master’s thesis on optical coherence tomography in the study of neurogenerative diseases. In 2018, she completed her doctorate under Friedemann Paul. The mother of two children remained part of Paul’s research team until her recent appointment.
Zimmermann hopes that optical coherence tomography will soon become standard in the diagnosis of MS. “Numerous studies that we have conducted with colleagues around the world indicate that it can tell us much more about the progression of the disease – and at a much earlier point in time.” Yet there is still work to do. “The method comes from ophthalmology. Clinicians from other disciplines must also acquire the necessary expertise to properly interpret the results of retinal analysis.”
Text: Catarina Pietschmann