Checkmating tumors
In chemotherapy, cytostatics – i.e., substances that are halting cell prolifieration – prevent cancer cells from growing and cause them to die. This approach often leads to success but has a number of drawbacks. It has a negative effect on healthy cells, and may also cause significant side effects in some patients. What’s more, in the case of very aggressive tumors, some cancer cells usually survive the therapy. “The remaining cancer cells are especially dangerous because they are altered in such a way that physicians often no longer know what type of cancer cells they are dealing with,” explains Dr. Gaetano Gargiulo, head of the Molecular Oncology research group at the Max Delbrück Center for Molecular Medicine in the Helmholtz Association (MDC). This makes it difficult to choose the right substances for further treatment.
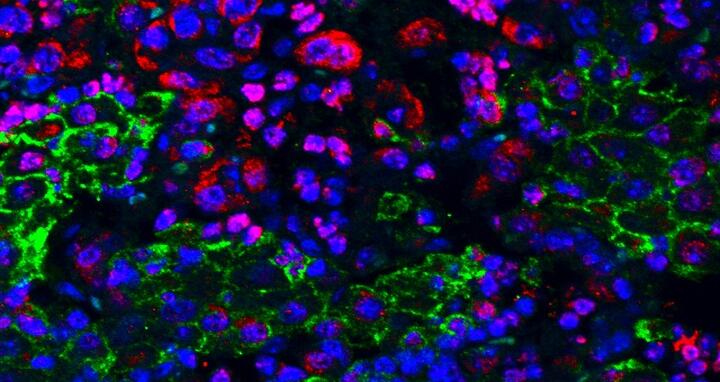
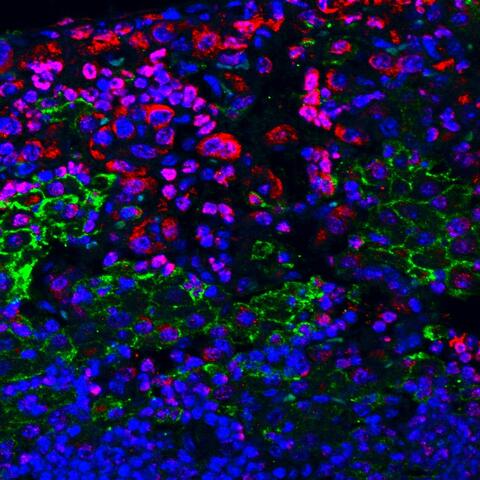
Microscopic image of tumor cells in which Ezh2 activity is inhibited (red) within a mouse lung and surrounded by immune cells (green)
Being prepared for the opponent’s next move
In a certain form of non-small cell lung cancer, the chemotherapy frequently results in altered cancer cells that are almost untreatable. Those developing new treatments must keep this possibility in mind. “Like a good chess player, we must think several moves ahead instead of just reacting to the present situation,” says Gargiulo. Together with his team and researchers under Professor Maarten van Lohuizen of the Netherlands Cancer Institute in Amsterdam, he has tested how this might work on mice that were injected with cells of a special form of non-small cell lung cancer.
In this form of non-small cell lung cancer, the cancer cells produce large quantities of an enzyme called Ezh2. The enzyme represses a number of tumor suppressor genes, which normally stop cells from multiplying out of control. Agents that inhibit this enzyme and thus reactivate the tumor suppressor genes are currently being tested in clinical studies. “In our mice, this agent initially worked as expected and inhibited the multiplication of tumor cells, thus keeping the cancer in check,” says Dr. Michela Serresi, the lead author of the publication and team leader associated with Gargiulo’s research group.
But the researchers had also expected the agent to lose its effect over time. “Interestingly, there always developed an inflammatory situation that in turn supported tumor growth,” says Serresi. The remaining cancer cells thus became even more aggressive as a result of the treatment.
Making cancer cells aggressive – and then moving in for checkmate
This is precisely where the MDC researchers are focusing their efforts. They are intentionally sending the tumor cells down this path – and setting them up for a trap. “Although the cells may be extremely aggressive once they are resistant to the Ezh2 inhibitor, they are dependent on the inflammatory situation,” explains Gargiulo. “If we can foresee this development, similar to the way skilled chess players think through the possible moves their opponents might make, and even deliberately force it to occur, we can also selectively combat it.” Therefore, in the second step of the therapy, the researchers administered the mice an anti-inflammatory substance – putting the cancer cells in checkmate.
However, it is still a long way to go before patients will see benefits from these new treatment strategies. “If we intentionally make cancer cells more aggressive, we have to know exactly what we’re doing,” says Gargiulo, adding that, for example, it would be necessary to search for biomarkers that enable clinical scientists to clearly predict in which patients this strategy will actually be effective. “We first have to gather sufficient data and experience in the lab before we can even think about testing this treatment strategy on patients,” emphasizes Gargiulo.
Reference
Michela Serresi et al. (2018): “Ezh2 inhibition in Kras-driven lung cancer amplifies
inflammation and associated vulnerabilities.” Journal of Experimental Medicine. doi:10.1084/jem.20180801
- The Max Delbrück Center for Molecular Medicine (MDC)
-
The Max Delbrück Center for Molecular Medicine in the Helmholtz Association (MDC) is one of the world’s leading biomedical research institutions. Max Delbrück, a Berlin native, was a Nobel laureate and one of the founders of molecular biology. At the MDC’s locations in Berlin-Buch and Mitte, researchers from some 60 countries analyze the human system – investigating the biological foundations of life from its most elementary building blocks to systems-wide mechanisms. By understanding what regulates or disrupts the dynamic equilibrium in a cell, an organ, or the entire body, we can prevent diseases, diagnose them earlier, and stop their progression with tailored therapies. Patients should benefit as soon as possible from basic research discoveries. The MDC therefore supports spin-off creation and participates in collaborative networks. It works in close partnership with Charité – Universitätsmedizin Berlin in the jointly run Experimental and Clinical Research Center (ECRC), the Berlin Institute of Health (BIH) at Charité, and the German Center for Cardiovascular Research (DZHK). Founded in 1992, the MDC today employs 1,600 people and is funded 90 percent by the German federal government and 10 percent by the State of Berlin.