MDC Scientists Reveal Role of Gene in Sensitivity to Thermal Pain
“As yet, c‑Kit is the first example of a single gene being required for normal noxious heat sensitivity of C‑fibers,” according to the neurobiologists. Their paper has just been published online in Neuron*.
Depending on the size of the individual, there are between 1.5 and 2 million sensory receptors in the skin which are sensitive to pain, pressure (touch) and temperature. These specialized sensory neurons, also called nociceptors, detect painful thermal and mechanical stimulation of the skin and transmit the information to the brain, where it is processed and consciously experienced as pain.
Dr. Alistair N. Garratt
“About 40 percent of the skin’s sensory receptors are responsible for the perception of pain,” Professor Lewin explained. “Receptors sensitive to touch account for only ten percent.” This disproportionate distribution of receptors specialized in pain and touch underscores the significance of pain sensitivity. “Without pain receptors,” Professor Lewin and Dr. Garratt pointed out, “we would quite probably die of unnoticed injuries at an early age.”
Pain threshold for heat is lowered
Pain receptors are nerve endings – nerve fibers that inform the brain about skin injuries. These nerve fibers have different cell surface receptors. One of these is c‑Kit, which the MDC researchers investigated more closely.
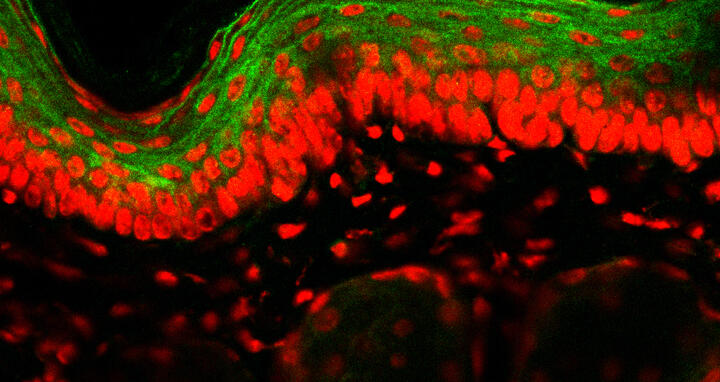
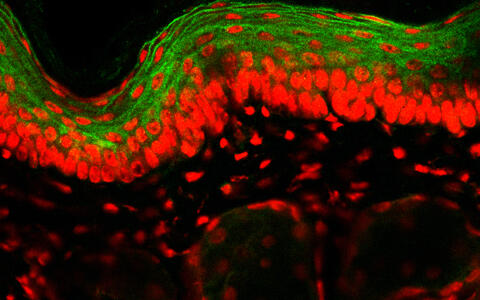
Cross-section of the skin: Stem Cell Factor (SCF) is located in the uppermost layer of the skin (marked green). According to MDC reseachers, SCF activates c‑Kit when the skin is injured. C‑Kit has now been identified as a gene related to heat-induced pain. The cell nuclei of the skin cells are marked red.
To study the characteristics of the receptor in more detail, the MDC researchers bred mice lacking c‑Kit. Experiments attempting this were already carried out in the 1950s, but the mice died of anemia very quickly. It was not until the advent of transgenic technology that this problem could be circumvented. Dr. Garratt administered the gene for erythropoietin (Epo) to the mice. Epo is a hormone which stimulates the production of red blood cells. As a result, the mice are no longer anemic and have a normal life expectancy.
Prof. Gary R. Lewin
If the mice – lacking c‑Kit but equipped with extra copies of the Epo gene – are exposed to temperatures that are normally extremely painful, they at first do not react. It takes a temperature of about 6 degrees Celsius (°C) above the normal pain threshold of approximately 41 — 50°C for the animals to respond to the stimulus. C‑Kit is activated by Stem Cell Factor (SCF), a ligand that it is expressed in the skin. Therefore, the scientists conclude that also when the skin is injured, SCF is released and stimulates c‑Kit, leading to a reduced pain threshold for heat. Consequently, sensitivity to heat in the affected area is elevated, as the MDC scientists observed after injection of SCF and measuring paw withdrawal latencies to a heat stimulus. Professor Lewin explained how this works. “It’s like having a sunburn – even lukewarm water becomes painful,” he said.
Cancer drug Gleevec (Imatinib) blocks c‑Kit – heat sensitivity decreases
The researchers attained similar results by administering Gleevec (imatinib), a drug that a few years ago revolutionized the treatment of breast cancer, leukemias and gastrointestinal stromal tumors, but also can apparently alleviate pain. Gleevec blocks a specific group of proteins to which c‑Kit also belongs.
In the experiments, sensory fibers of wild-type mice expressing c‑Kit that were given Gleevec showed the same properties as those of mice that did not express c‑Kit: the pain threshold for heat was clearly higher in wild-type mice treated with Gleevec. They were able to bear higher temperatures than the control mice not given Gleevec. Next, the researchers want to investigate if Gleevec really can alleviate pain in patients.
*Nociceptive tuning by Stem Cell Factor/c‑Kit signaling
Nevena Milenkovic1,3, Christina Frahm1,3, Max Gassmann², Carola Griffel1, Bettina Erdmann1, Carmen Birchmeier1, Gary R. Lewin1,*, Alistair N. Garratt1,*
1Max Delbrueck Center for Molecular Medicine,Berlin, Germany;
2Vetsuisse Faculty and Zurich Center for Integrative Human Physiology, Zurich, Switzerland
3authors contributed equally
Barbara Bachtler
Press and Public Affairs
Max-Delbrück-Center for Molecular Medicine (MDC) Berlin-Buch
Robert-Rössle-Straße 10; 13125 Berlin; Germany
Phone: +49 (0) 30 94 06 — 38 96
Fax: +49 (0) 30 94 06 — 38 33
e‑mail: presse@mdc-berlin.de
http://www.mdc-berlin.de/englisch/about_the_mdc/public_relations/e_index.htm