Angiotensin II Type 1‑Receptor-Activating Antibodies in Renal-Allograft Rejection
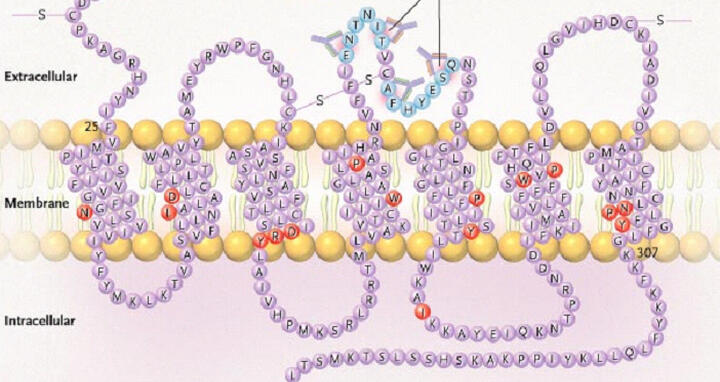
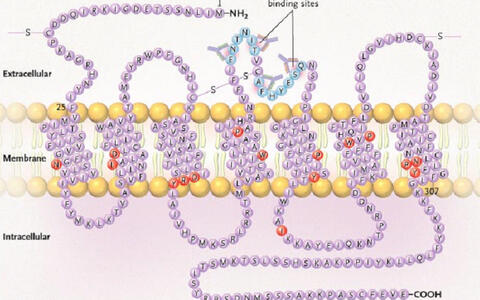
The association between HLA antibodies present at the time of transplant and graft loss has been well established. Now, Duska Dragun, Dominik Müller, Gerd Wallukat and their colleagues report that a non-HLA, angiotensin II type 1 (AT1)- receptor meditated pathway may be involved in kidney transplant rejection (New England Journal of Medicine 2005; 352: 558 – 69).
The scientists studied 33 kidney transplant recipients who presented with antibody-mediated rejection following kidney allograft. Of these, 13 had donor-specific anti-HLA antibodies. Sixteen of the remaining 20 patients without anti-HLA antiobodies were shown to have both agonistic antibodies targeting the AT1- receptor and malignant hypertension. Furthermore, when agonistic antibodies were transferred to rats that had received kidney transplants, hypertension and vasculopathy were induced.
Of the 16 patients with agonistic antibodies, seven underwent plasmapheresis for the removal of the antibodies and received the AT1- receptor blocker losartan. As compared to those control patients who received standard treatments, these seven fared better in terms of renal function and graft survival. Thus, novel therapies for the treatment of antibody-mediated rejection may be developed that involve the removal of AT1- receptor antibodies or the blockage of AT1 receptors.
Duska Dragun obtained her doctoral degree at the Franz Volhard Clinic (MDC) and is now at the Charite University Hospital. Dominik Müller leads a group at the Franz Vollhard Clinic that studies the molecular mechanisms of the pathogenesis of hypertension/angiotensin II-induced cardiac, renal, and vessel damage. Gerd Wallukat heads a group at the MDC researching immunological mechanisms of cardiac injury.
Contact:
Pamela Cohen
p.cohen@mdc-berlin.de
+49 30 9406 2121