Kick-starting the kidneys with an established antifungal drug
For people suffering from diabetes insipidus, everyday life can be a struggle: Not only do they produce up to 20 liters of urine every day, they also have to drink just as much. This rare disorder, in which the kidneys do not absorb enough water from urine, can be inherited, but it can also be triggered later in life by factors such as medication.
In the future, diabetes insipidus patients could find help in the form of an antifungal drug called fluconazole. Research teams led by Dr. Enno Klußmann and Professor Kai Schmidt-Ott at the Max Delbrück Center for Molecular Medicine (MDC) published their recent findings in the Journal of the American Society of Nephrology. The article explains the effect the drug has on the kidneys, but also why it is not suitable for everyone with the condition.
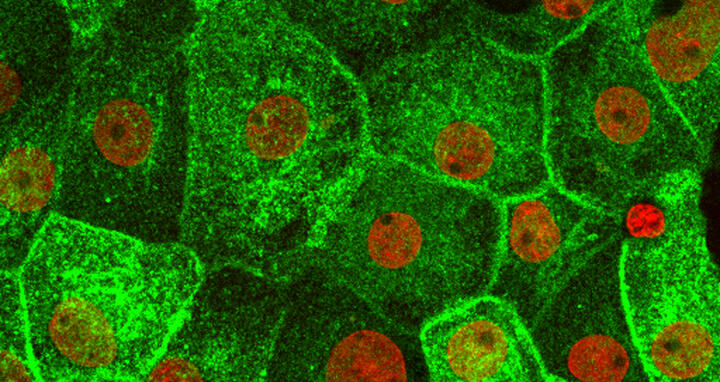
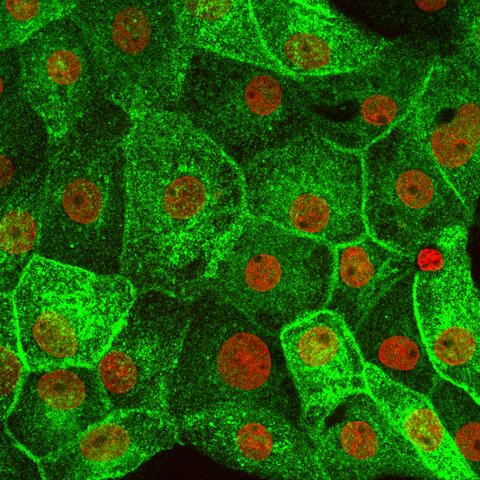
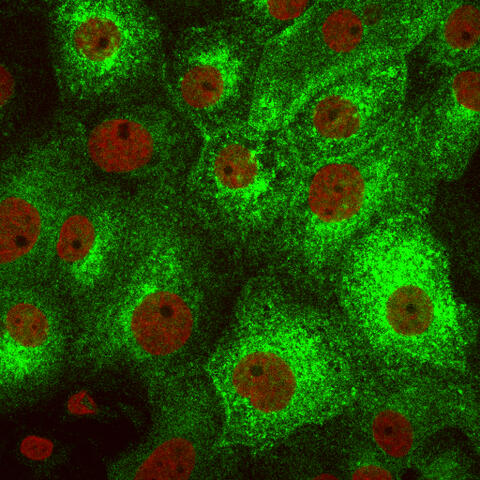
In rat kidney cells, green-labelled aquaporin AQP2 partially migrates to the cell surface as soon as it is stimulated by the drug forskolin. Cell nuclei appear red.
Fluconazole helps the body reabsorb more water
The drug works by activating tiny water channels (aquaporins) in specialized cells within the collecting ducts of the kidney. Once activated, they form pores in the cell surface through which water molecules can flow. This way, the kidneys are able to transport water from the urine back into the body.
Normally, this process is very meticulously controlled by the hormone vasopressin. “But if the hormone is absent or cannot act on the cell, this can lead to massive loss of free water into the urine,” says Dr. Christian Hinze, scientist at kidney specialist Schmidt-Ott’s lab at the MDC. “Fluconazole can trigger this function without the hormone, to some extent.”
Hinze and his colleague Dr. Tanja Vukićević demonstrated that fluconazole can restore about 30 percent of normal water reabsorption in mice whose vasopressin hormones have been blocked by a different agent.
The green-labelled aquaporin AQP2 is found in the kidney cells of the rat inside the cells if they have not been stimulated either by the hormone or by a drug. Cell nuclei appear red.
One size does not fit all
These experiments enable scientists to better assess whether the substance has the potential to become a new therapeutic agent for humans. “Fluconazole is only effective if the aquaporin mechanisms in the kidney cells are still intact,” says Klußmann. Patients with aquaporin gene mutations, for example, may not benefit from future fluconazole treatment.
The drug signals hope for patients whose bodies produce too little vasopressin due to genetic factors, or whose kidney cells are insensitive to the hormone due to a mutation in the hormone receptor. Excess water excretion also affects about half of those who take lithium as medication. As this is the result of the kidneys no longer reacting sufficiently to the hormone, they too could potentially benefit from fluconazole.
How the cells of the kidney’s collecting ducts are affected
“Human kidneys produce 180 liters of primary urine every day,” says Hinze. “In the end, however, only a few liters per day should be excreted as secondary or final urine.” This is because the tiny tubes that channel the urine into the renal pelvis draw water from the liquid in the exact quantities required. The final sections of these tubes, the collecting ducts, serve a crucial role in the hormone-controlled fine tuning of this process.
And it’s here that the repurposed drug comes into play. MDC researcher Tanja Vukićević cultivated collecting duct cells from rats in a petri dish, and analyzed in detail the effect of the antifungal drug. Her experiments showed that aquaporin molecules migrate to the surface of the cell under the influence of the drug. A team of colleagues from Kiel University prepared the tiny collecting ducts from the kidneys of mice, and were able to show that fluconazole improves water transport.
Next step: clinical trials
Back in 2013, scientists led by Klußmann already discovered in a large-scale screening test that fluconazole influences the localization of aquaporins.
As a next step, the researchers are planning to conduct a study on a handful of human test subjects. Only then will we know whether the drug also has the desired effect in humans. “The efficacy and tolerance of such a treatment remains to be seen,” says Klußmann, who is planning the clinical trial together with his colleagues. “But even if it helps only a few people, it will have been worth the effort.”
Original publication
Tanja Vukicevic, Christian Hinze, et al. (2019): “Fluconazole Increases Osmotic Water Transport in Renal Collecting Duct through Effects on Aquaporin‑2 Trafficking”, J Am Soc Nephrol 30. doi:10.1681/ASN.2018060668