Fratricide among T cells
One of the most promising new approaches in the fight against cancer is the attempt to train a patient’s own immune system to fight a tumor. White blood cells called T cells play a key role in immunity against viruses and parasites, and researchers hope to train them to combat tumors as well. The idea is to isolate T cells from a patient’s blood, outfit them with molecules that recognize cancerous cells, grow them quickly in the lab, and reintroduce them into the patient’s body. Wolfgang Uckert’s lab at the MDC, collaborating with Dolores J. Schendel’s lab at the Helmholtz Center in Munich, has now clarified one of the problems in doing so. Their work appeared in a recent issue of the Journal of Clinical Investigation.
Human T cells are capable of recognizing billions of molecules – including those of disease agents, and potentially those of a tumor – because as the body produces each cell, it is outfitted with a unique T cell receptor (TCR). These versatile molecules are able to detect certain protein fragments (antigens) bound to a complex of proteins called the major histocompatibility complex (MHC) on the surface of other cells. MHCs are found in different types in the human population – an important point for later – but within a single person they are identical, and appear on almost every cell in the body. If a cancer antigen can be recognized by a TCR created in the lab, this opens the door to a therapeutic approach called TCR gene therapy. Here, genes encoding for tumor-specific TCR are used as off-the-shelf reagents to render every patients’ T cells tumor-reactive. The labs of Wolfgang and Dolores are using their expertise to generate T cells that recognize tumor antigens in order to investigate their potential for clinical use.
A central problem in this effort is that a therapeutic TCR has to target an antigen which is specific to the tumor; in other words, it shouldn’t be found on healthy cells that should remain untouched by the treatment. A major difficulty in this pursuit is the fact that cancer arises from a person’s own cells and mostly resembles his or her own tissue; therefore, suitable tumor antigens have been difficult to identify. However, as tumors develop, they acquire various mutations and produce abnormal amounts of certain proteins. Those might serve as antigens that could target the tumor for an attack by T cells.
Recently, the U.S. National Cancer Institute launched a project to identify tumor antigens that showed promise for use in immune therapies. One molecule, a human protein called survivin, was given a high ranking because it appears frequently in aggressive tumor cells and is believed to be rare in healthy tissues. Its role in tumor cells is to protect them from self-destruction, which is the fate of most cells in the body that suffer from defects. Matthias Leisegang from Wolfgang’s group, working with Susanne Wilde from Dolores J. Schendel’s lab, decided to use survivin as the basis for studying the ability of T cells to specifically recognize cancer cells.
Matthias, Susanne and their colleagues were able to grow T cells in the lab that had TCRs capable of recognizing an antigen derived from the survivin protein and presented by an MHC molecule called HLA-A2. If they transferred the TCR genes into T cells of other individuals, these cells showed therapeutic potential, because they were capable of eliminating tumor cells and expanding to sufficient numbers. However, this was only achieved if the T cells were derived from an individual who does not express HLA-A2. But things got problematic when they tried to mimic the clinical situation and transferred the TCR genes into T cells which did express HLA-A2. Surprisingly, the cells died as they were being cultured in the lab.
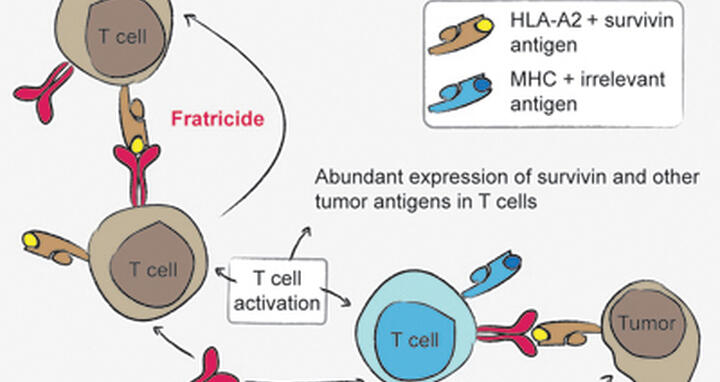
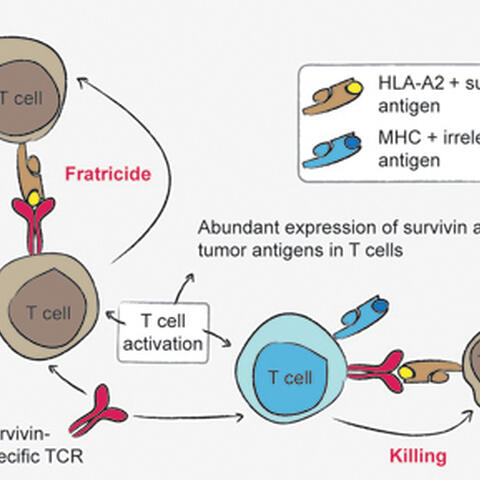
Additional experiments revealed the reason: as T cells multiply, they produce high amounts of survivin themselves, making them just as much targets of the therapy as the tumor. Matthias and Susanne discovered that this causes the cells to kill each other – to commit “fratricide” – if they are of a compatible MHC type. The process can be seen as a drastic form of autoimmunity. “Obviously this would be an obstacle to therapy,” Wolfgang Uckert says. “The same thing would happen if these cells were being used in a treatment. If we start with a patient’s own cells and train them to recognize survivin, they’ll do so. But before they multiply enough to destroy cancer cells bearing survivin, they will be destroyed themselves.”
Uncovering this case of fratricide sheds light on the attempt to find antigens that will make suitable targets in cancer therapies involving T cells. In their work, the investigators analyzed the appearance of other prominent tumor antigens in T cells; their results indicated that some of these antigens might also lead to T cell-mediated fratricide. “The whole idea is to activate the patient’s immune system against diseased tissue produced by his or her own body, which means the cells will inevitably be of the same MHC type,” Wolfgang summarizes. “In doing so, a therapy has to walk a very fine line, because it can’t be turned loose on healthy tissue such as T cells. A tumor cell has to look just different enough to be targeted without that happening. This experiment shows that it may be more difficult than we had hoped. But we are hopeful that the results may be different with other tumor markers.” The outcome of this work underlines the importance of selecting the right antigens as targets in the design of successful therapies utilizing the body’s own immune cells.
- Russ Hodge
Highlight Reference:
Leisegang M, Wilde S, Spranger S, Milosevic S, Frankenberger B, Uckert W, Schendel DJ. MHC-restricted fratricide of human lymphocytes expressing survivin-specific transgenic T cell receptors. J Clin Invest. 2010 Nov 1;120(11):3869 – 77.