Taking out the cellular trash
If we don’t take out the trash regularly, our homes become unpleasant and even a danger to our health. The same applies to our cells: If excess proteins and strands of genetic material aren’t removed, the cell and ultimately the entire organism can fall ill. For instance, scientists suspect there is a connection between Alzheimer’s and mutations that cause defects in cellular garbage removal. What’s more, tests with mice have shown that suppressing the breakdown of DNA and RNA can trigger serious autoimmune diseases.
But concrete evidence is missing: “There’s a lot of research showing how genetic information in the form of DNA and RNA is produced in humans. But there’s less knowledge about how waste DNA and RNA are removed,” says Professor Oliver Daumke, a lab leader at the Max Delbrück Center. To address this, he teamed up with researchers from Kiel University to examine waste removal in cells in more detail. Their work focused on an enzyme called PLD3, which is responsible for breaking down waste. The researchers began by determining its structure using a crystal structure analysis. They were able to identify specific segments that play a key role in breaking down RNA and DNA. “That gave us a better understanding of how the waste is broken down and of the morbid effects of mutations in the PLD3 protein,” says Daumke.
Mutations in the PLD3 gene raise Alzheimer’s risk
PLD3 belongs to a protein family of enzymes that normally break down cellular fats in human cell organelles known as lysosomes. In humans, PLD3 is produced by a gene of the same name. “We’ve been looking at the PLD3 gene for some time already, because it became clear a few years ago that mutations in the gene could be involved in the development of Alzheimer’s,” says Professor Markus Damme of Kiel University. “Our work, as well as work by other researchers, showed that PLD3 actually breaks down DNA and RNA instead of fats,” he says.
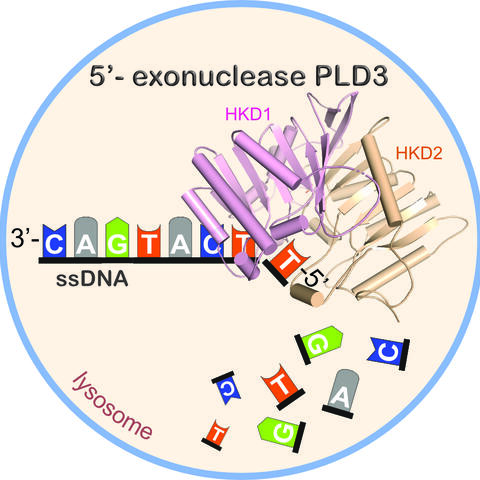
The PLD3 protein cleaves individual nucleic acid building blocks (A, T, G, C) from short single-stranded DNA. This process takes place within the catalytic active center of the enzyme, which consists of two structural subunits (HKD and HKE).
“But it wasn’t clear how this was happening,” says Cedric Cappel, a researcher in Damme’s group and co-lead author of the paper. “So we decided to examine the protein’s structure more closely – in the hope that we could learn something about its link to Alzheimer’s.” Cappel made some of the protein and sent it to Dr. Yvette Roske, a structural biologist in Daumke’s lab and the other co-lead author of the paper. She succeeded in producing tiny crystals of PLD3. Exposing the crystals to X‑rays produces a diffraction pattern that made it possible to reconstruct the protein’s structure. Roske could then depict the crystal structure with and without a bound RNA, and analyze it. “We found that two of these proteins combine to form something called a dimer. We haven’t seen that happen among other enzymes in this family,” says Roske. But why do the proteins do this? “It could be because the protein is only stable in a pair,” says Cappel. “Alone, it would probably be broken down.”
Through their work, these two research groups have provided the first structural proof of DNA and RNA being broken down by PLD3. “Now we can gain a rough understanding of the reaction mechanism,” says Roske. The researchers also found two areas of the protein that could be key to its functioning and presumably altered in Alzheimer’s patients – an early indication of a possible disease mechanism.
“Our research has provided a map of the protein,” says Cappel. Future studies of PLD3 can use this map to answer questions such as which areas are key to the functioning of PLD3, and what happens when changes are made to these areas. The researchers hope this will lead to a better understanding of the role the protein plays in certain diseases. This knowledge would then potentially make it possible to take corrective action.
Text: Janosch Deeg
Further information
Literature
Yvette Roske, et al. (2023): “Structural analysis of PLD3 reveals insights into the mechanism of lysosomal 5’-exonuclease-mediated nucleic acid degradation”, in Nucleic Acids Research, DOI: 10.1093/nar/gkad1114
Contacts
Christina Anders
Editor, Communications Department
Max Delbrück Center
+49-(0)30 – 9406-2118
christina.anders@mdc-berlin.de or presse@mdc-berlin.de
- Max Delbrück Center
The Max Delbrück Center for Molecular Medicine in the Helmholtz Association (Max Delbrück Center) is one of the world’s leading biomedical research institutions. Max Delbrück, a Berlin native, was a Nobel laureate and one of the founders of molecular biology. At the locations in Berlin-Buch and Mitte, researchers from some 70 countries study human biology – investigating the foundations of life from its most elementary building blocks to systems-wide mechanisms. By understanding what regulates or disrupts the dynamic equilibrium of a cell, an organ, or the entire body, we can prevent diseases, diagnose them earlier, and stop their progression with tailored therapies. Patients should be able to benefit as soon as possible from basic research discoveries. This is why the Max Delbrück Center supports spin-off creation and participates in collaborative networks. It works in close partnership with Charité – Universitätsmedizin Berlin in the jointly-run Experimental and Clinical Research Center (ECRC), the Berlin Institute of Health (BIH) at Charité, and the German Center for Cardiovascular Research (DZHK). Founded in 1992, the Max Delbrück Center today employs 1,800 people and is 90 percent funded by the German federal government and 10 percent by the State of Berlin.