The immune system is almost always involved
Immune cells are everywhere in the human body. “It was previously believed that the brain, at least, was a kind of no-go zone for the immune system,” says Prof. Klaus Rajewsky, head of the research group on Immune Regulation and Cancer at the Max Delbrück Center for Molecular Medicine (MDC). But this belief was a serious misconception. “All important diseases of the central nervous system, such as Alzheimer’s or Parkinson’s, have a strong immunological component,” emphasizes Rajewsky. “And by now, we actually believe there is hardly any human disease that does not involve the immune system.”
This is one of the reasons why more and more scientists are focusing on immunology. “It is a highly explosive field of research,” says Rajewsky, who is also a member of the steering committee of the Helmholtz research initiative Immunology & Inflammation – or I&I for short. Since 2017, this project has seen a total of 23 working groups join forces from the five Helmholtz Centers in Berlin, Bonn, Hanover, Heidelberg, and Munich. Together, they hope to answer immunology’s most current and important questions. Rajewsky is sure that, in the next ten years, medicine will be drastically altered by immunotherapies.
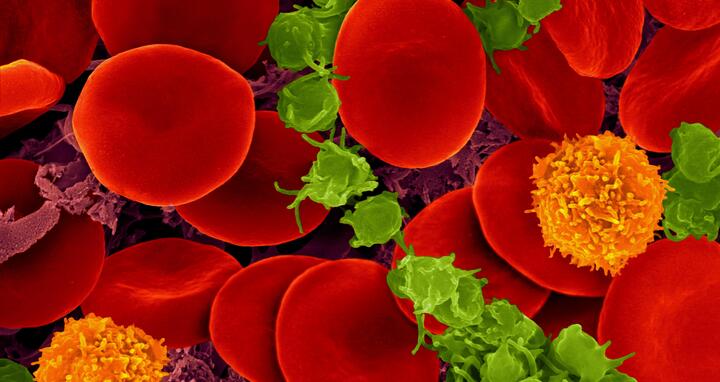
Human blood with red blood cells, T cells (orange) and platelets (green)
Repairing defective T cells in children
In mid-September, the German Society for Immunology (DGfI) and the Italian Society of Immunology, Clinical Immunology and Allergology (SIICA) held a four-day conference in Munich to discuss the latest developments in this field of research. During the conference, Prof. Ellen Renner from Helmholtz Zentrum München and Prof. Tim Niehues, chief physician at the Center for Pediatrics and Adolescent Medicine at Helios Hospital Krefeld, organized a satellite I&I symposium in coordination with Rajewsky.
“We had great speakers and welcomed at least 200 guests, maybe more,” reports Rajewsky, who spoke himself at the symposium about his attempts to help children suffering from congenital T-cell defects. Such defects may mean, for example, that their immune cells are unable to fight the widespread Epstein-Barr virus. Children infected with this virus are at higher risk of life-threatening diseases – which is why most of these young patients die early.
“Our idea is to correct the genetic defect using gene editing – either in the T cells themselves or in the hematopoietic stem cells from which the T cells originate,” explains Rajewsky. To do this, the researcher and his team use the CRISPR-Cas9 method, now commonly known as “gene scissors.” “So far, the results we have achieved with mouse models and with isolated human T cells are very encouraging,” says the immunologist.
Targeted help for an immobilized immune system
Prof. Dirk Busch from the Institute for Medical Microbiology, Immunology and Hygiene at the Technical University of Munich (TUM) also spoke at the symposium about the manipulation of T cells. The method that Busch and his team are currently developing is intended for patients whose own immune system has been temporarily immobilized – for example, by a bone marrow transplant in the treatment of a tumor.
Patients are left particularly susceptible to infection while the hematopoietic system is being rebuilt. Busch’s idea is that, during this phase, the patients receive modified T cells – ideally gained by using gene editing techniques to equip the patient’s own T cells with a new receptor. This would specifically target viruses such as cytomegalovirus (CMV). CMV is a very common virus that does not usually cause symptoms in healthy people. For patients with a weakened immune system, however, it can be life-threatening.
As Busch discussed at the event, due to their rapid proliferation, the administration of very few modified T cells – in extreme cases, even of a single cell – can be sufficient to effectively combat CMV infections in immunocompromised patients. The researcher has developed an entire library of receptors that target different clinically relevant viruses. Rajewsky says that his colleague’s method is currently still being tested in clinical trials, but he is sure that it will be widely used in the foreseeable future.
Basic researchers and clinicians exchange ideas and experiences
Prof. Eicke Latz from the German Center for Neurodegenerative Diseases (DZNE) in Bonn and director of the Institute for Innate Immunity at the University of Bonn spoke at the symposium about the influence of nutrition on inflammatory processes in the body. Latz has discovered an important metabolic pathway that is triggered by a diet rich in fat and protein – a common diet in Germany – and that influences the myeloid cells of the immune system in such a way that they may promote inflammatory diseases. This opens up new preventive and therapeutic possibilities.
Prof. Hans-Reimer Rodewald from the German Cancer Research Center (DKFZ) in Heidelberg also spoke at the I&I symposium. He talked about how different immune cells in the body develop from stem cells to form and maintain a functional immune system – for example, following major blood loss. In his most recent work, Rodewald succeeded in equipping immune system cells with a “bar code system,” which then allowed him to track their movement in the living organism. Using this method, scientists can research how the multitude of different cell types are created in the blood.
“In summary – and without being able to go into all the contributions here – I can report that the guests were very happy with our symposium,” says Rajewsky. “It brought together basic researchers and clinicians, and everyone was able to have useful and pleasant exchanges.”
Robin Graf
The Otto Westphal PhD Prize goes to Robin Graf of the MDC
And there were even more reasons for Rajewsky to be pleased with the DGfI conference: Two researchers from the MDC were awarded coveted prizes in Munich. The €1,500 Otto Westphal PhD Prize went to Dr. Robin Graf from Rajewsky’s research group. The jury praised his outstanding dissertation, which investigates the relevance of the B-cell receptor in the development of B1 cells.
These particular cells, which belong to a class of white blood cells called lymphocytes, are the only cells in the immune system capable of making antibodies. With his most important study, which was published in the journal Science in February of this year, Graf, together with other researchers from Rajewsky’s group, was able to show that the B-cell receptor plays an instructive role in the development of B1 cells. B1 cells are believed to play an important role in natural immunity – i.e., the innate immune system. B2 cells, on the other hand, are mainly responsible for adaptive immunity.
Dr. Kathrin de la Rosa
Also honored was MDC researcher Kathrin de la Rosa
Dr. Kathrin de la Rosa (née Pieper), who since July 2018 has headed the MDC research group on Immune Mechanisms and Human Antibodies, received the Fritz and Ursula Melcher Postdoctoral Prize, which also comes with €1,500. As a researcher in Prof. Antonio Lanzavecchia’s lab at the Swiss Federal Institute of Technology (ETH) in Zurich, the researcher described a new and completely unexpected molecular mechanism of antibody diversity in two papers published in the journal Nature.
Dr. de la Rosa and her colleagues discovered an antibody with a special property: It “steals” a segment of the B cell gene called LAIR, which is located on a chromosome that doesn’t contain any blueprints for antibodies. This trick enables the antibody to gain an extra domain, allowing it to recognize the different variants of the malaria pathogen Plasmodium falciparum. It is thus, the jury said in its statement, a new tool for fighting malaria and a promising candidate for developing a vaccine.
Text: Anke Brodmerkel
Further information