Towards a better understanding of heart failure
When the heart is unable to supply the body with enough blood – and hence oxygen and nutrients – to meet the body’s demand, this is known as heart failure. Common symptoms of heart failure include shortness of breath, fatigue upon exertion, chest tightness and swollen legs. The condition, which currently affects approximately four million people in Germany, is one of the most common reasons for hospital admission. Heart failure bears a poor prognosis, and up to 50 percent of patients will die from the disease within five years.
Heart failure is currently subdivided into two different types, regardless of the condition’s underlying cause. When the heart muscle is no longer strong enough to pump sufficiently, the patient develops what is known as ‘Heart Failure with reduced Ejection Fraction’ (HFrEF). This contrasts with ‘Heart Failure with preserved Ejection Fraction’ (HFpEF), a condition in which the heart contracts efficiently, but its ventricles are too stiff to properly fill with blood. Approximately half of all individuals with heart failure have HFpEF. This latter type of heart failure is the focus of the new Collaborative Research Center (SFB), which sees Charité collaborate with the Max Delbrück Center for Molecular Medicine (MDC), Freie Universität Berlin (FU), the German Heart Center Berlin (DHZB) and Hannover Medical School (MHH). The German Research Foundation (DFG) is funding the alliance with around 12 million euros for an initial period of four years.
The new SFB led by the Charité investigates heart failure with preserved ejection fraction — a specific form of cardiac insufficiency — as a systemic, heterogeneous clinical picture.
The most important underlying causes responsible for both HFpEF development and progression are common risk factors and comorbidities such as high blood pressure and diabetes – associated with increased body weight, smoking and sedentary lifestyle. HFpEF mainly affects the elderly, and more women than men. Given current trends in demographics, we will likely see an increase in cases over time. In contrast to patients with HFrEF, the other type of heart failure, patients with HFpEF still have very little access to effective and causal treatment.
Eight MDC research groups are involved
Eight research groups from the MDC are involved in the Collaborative Research Center: the groups of of Professor Michael Gotthardt, Professor Norbert Hübner, Professor Holger Gerhardt, Dr. Suphansa Sawamiphak, Dr. Sofia Forslund, Dr. Paolo Annibale, Dr. Philipp Mertins and the group of Professor Dominik Müller und Professor Ralf Dechend.
“Heart failure with preserved ejection fraction is a systemic disorder – that is, it affects the entire body. Sadly, our knowledge of the disease’s basic mechanisms and cardiovascular changes remains extremely limited. This means we are still not in a position to offer specific treatments to the large group of patients with HFpEF,” explains the new SFB’s spokesperson, Professor Burkert Pieske, Head of the Department of Internal Medicine and Cardiology on the Charité Campus Virchow-Klinikum. “We would like our new research endeavor to remedy that. Our aim is to produce a comprehensive description and classification of what is a systemic and heterogeneous condition in order to improve our understanding of HFpEF and our ability to treat it. We will do this on multiple levels. In addition to looking at the body as a whole and at individual organs, we will conduct research at both the molecular and cellular levels,” explains Professor Pieske.
© Max-Delbrück-Center
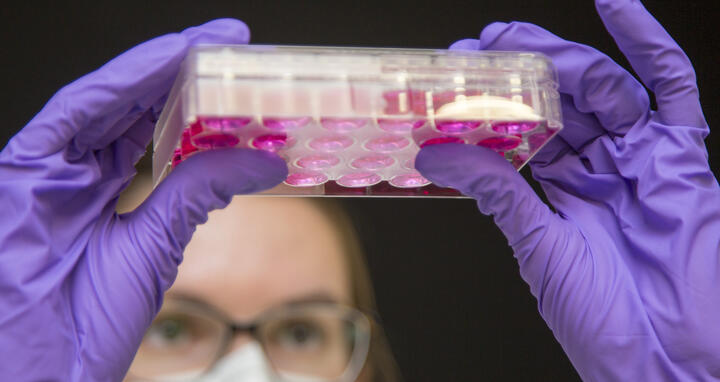
Michael Gotthardt and his team have been researching heart failure since several years – including the role of the giant protein titin in cardiac filling. Recently, they have found a compound that makes the heart muscle cells more elastic – a first step towards a possible therapy approach. In the Collaborative Research Center, Michael Gotthardt will now investigate how biomechanics and signal transduction are interconnected – with a special focus on gender-specific differences in disease progression. Michael Gotthardt is the deputy spokesman of the Collaborative Research Center. Furthermore, he provides the participating groups with the infrastructure to generate and analyze artificial heart tissue. This way, the researchers hope to reduce the number of animal experiments throughout the Collaborative Research Center.
Probing into the mechanisms of HFpEF
Conducted by an interdisciplinary team of experts from basic, translational, and clinical research including computational modeling, this endeavor will follow a multilevel approach. Believing that the disruption of specific signaling pathways is responsible for the development of distinct molecular HFpEF phenotypes with different characteristics, the researchers will study the mechanical, metabolic, inflammatory, and immunological factors responsible for disease development and progression. In each case, they will also study the downstream signaling pathways and the specific effects these might exert on the cardiovascular system.
Michael Gotthardt’s lab provides the participating research groups with the infrastructure to generate and analyze artificial heart tissue.
The researchers will be able to draw on their expertise in translational cardiology, functional genomics, cell and molecular biology, systems medicine, bioinformatics, and artificial intelligence. The MDC contributes its expertise in proteomics and single cell analyses to facilitate the analysis of complex systems at the molecular and cellular level. This approach is complemented by using state-of-the-art imaging technologies, phenotypic analysis and computer-based modeling. Summarizing the aims of their research, Professor Pieske says: “We want to develop a classification system for patients with heart failure with preserved ejection fraction which will enable us to use both molecular and clinical features to produce clear case definitions and diagnoses. We hope that this will one day enable us to offer patients a more personalized and targeted approach to treatment.”
Text: Charité / MDC